Respiratory Infections in Care Settings: Prevention and Early Intervention
Respiratory infections spread quickly in care homes. Learn how prevention, early warning signs, and rapid GP care protect residents’ health.
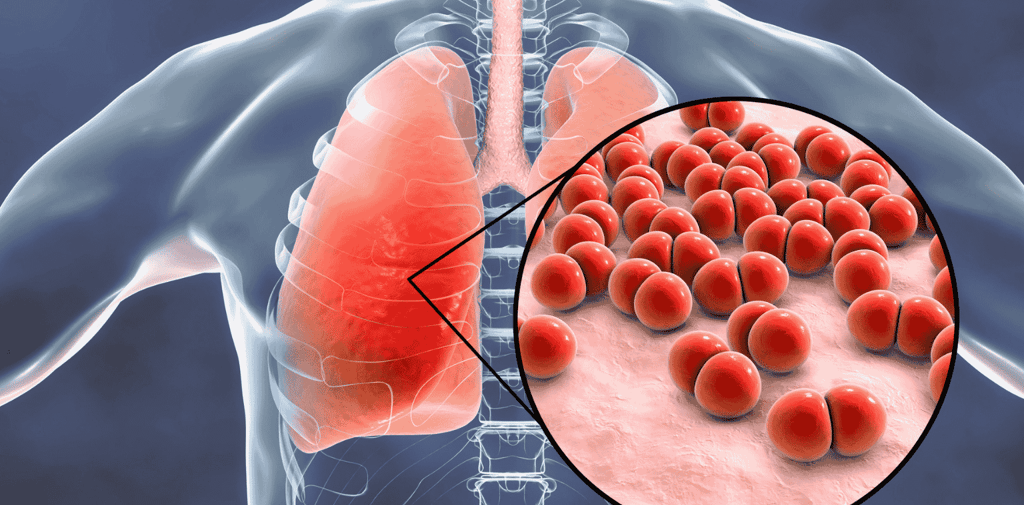
Respiratory infections are among the most common and dangerous health threats facing care home residents. From seasonal flu to pneumonia, these infections spread rapidly in communal settings and can quickly become life-threatening in elderly individuals with weakened immune systems.
Effective prevention strategies combined with early intervention when infections do occur can dramatically reduce serious complications and save lives.
Why Care Homes Are High-Risk Environments
Care homes create perfect conditions for respiratory infection transmission: close living quarters facilitating person-to-person spread, residents with compromised immune systems, multiple chronic conditions reducing infection-fighting capacity, and frequent visitor traffic introducing new pathogens.
Understanding these vulnerabilities emphasizes why prevention and early intervention aren't optional—they're essential components of responsible care.
Prevention: The First Line of Defense
Preventing respiratory infections is far more effective than treating them after they develop.
Essential prevention strategies:
Annual flu vaccinations for all residents and staff
Pneumonia vaccinations as recommended
Rigorous hand hygiene practices by staff and visitors
Respiratory etiquette (covering coughs, disposing tissues properly)
Adequate ventilation throughout living spaces
Isolating residents with confirmed infections when possible
Staff staying home when symptomatic
These simple measures, implemented consistently, significantly reduce infection rates and protect vulnerable residents.
Recognizing Early Warning Signs
Early detection allows prompt treatment before infections become severe.
Key respiratory infection symptoms:
New or worsening cough
Increased breathlessness or rapid breathing
Fever or feeling unusually cold
Confusion or increased disorientation (often the first sign in elderly)
Reduced appetite or general malaise
Chest pain or tightness
Increased sputum production or colour changes
In elderly residents, particularly those with dementia, subtle behavioural changes often indicate infection before obvious respiratory symptoms appear. Any unexplained deterioration warrants immediate medical assessment.
The Danger of Diagnostic Delays
Respiratory infections progress rapidly in frail elderly individuals. What begins as a mild cold can become pneumonia within 24-48 hours if left untreated.
Complications of delayed treatment:
Simple chest infections becoming severe pneumonia
Respiratory failure requiring hospitalization
Sepsis from overwhelming infection
Exacerbation of existing conditions like COPD or heart failure
Increased mortality risk
This is precisely why out-of-hours and weekend GP support matters critically. Respiratory symptoms don't wait for Monday morning appointments, and same-day assessment can prevent a manageable infection from becoming a medical emergency.
Effective Early Intervention
When respiratory infections are identified early, prompt treatment prevents serious complications.
Key intervention components:
Medical assessment:
Rapid GP evaluation determining infection severity
Chest examination and oxygen saturation monitoring
Decision whether antibiotics are appropriate
Assessment of hospitalization need
Treatment initiation:
Same-day prescription delivery ensuring antibiotics start immediately
Appropriate pain and fever management
Increased fluid intake and rest
Oxygen therapy if required
Monitoring:
Regular vital signs checking
Watching for deterioration requiring escalated care
Follow-up GP review ensuring improvement
Telehealth consultations allow initial assessment, with onsite GP visits available when physical chest examination is needed.
Managing Residents with Chronic Respiratory Conditions
Residents with COPD, asthma, or other chronic lung conditions require extra vigilance during infection season.
Special considerations:
Ensuring rescue inhalers are readily accessible
Earlier antibiotic intervention than in healthier individuals
Lower threshold for hospital referral if deteriorating
Ensuring regular medications continue during acute illness
When Hospital Admission Becomes Necessary
Despite best efforts, some respiratory infections require hospital treatment: severe breathlessness, oxygen saturation below 90%, signs of sepsis, inability to take oral medications, or no improvement after 48 hours of antibiotics all warrant hospital transfer.
Private ambulance services ensure safe transport when emergency services aren't required but hospital assessment is necessary.
The Role of Comprehensive GP Support
Effective respiratory infection management requires accessible, expert medical oversight.
Essential GP service features:
Rapid response to suspected infections (within hours, not days)
Availability during evenings and weekends when symptoms often worsen
Both telehealth and onsite assessment options
Immediate prescription access through same-day delivery
Follow-up monitoring ensuring infections resolve completely
The Bottom Line
Respiratory infections in care settings require proactive prevention combined with rapid intervention when infections occur. The window between early infection and serious complications is often measured in hours, not days.
Care homes with comprehensive GP partnerships offering out-of-hours support, rapid assessment, and same-day prescriptions can manage respiratory infections effectively, keeping residents safe and avoiding preventable hospital admissions. Your parent deserves this responsive, expert care when respiratory infections threaten their health.


