Diabetes Care in Residential Settings: Beyond Blood Sugar Monitoring
Diabetes care in care homes goes beyond blood sugar checks. Learn how medication, nutrition, foot care, and GP support protect residents’ health.
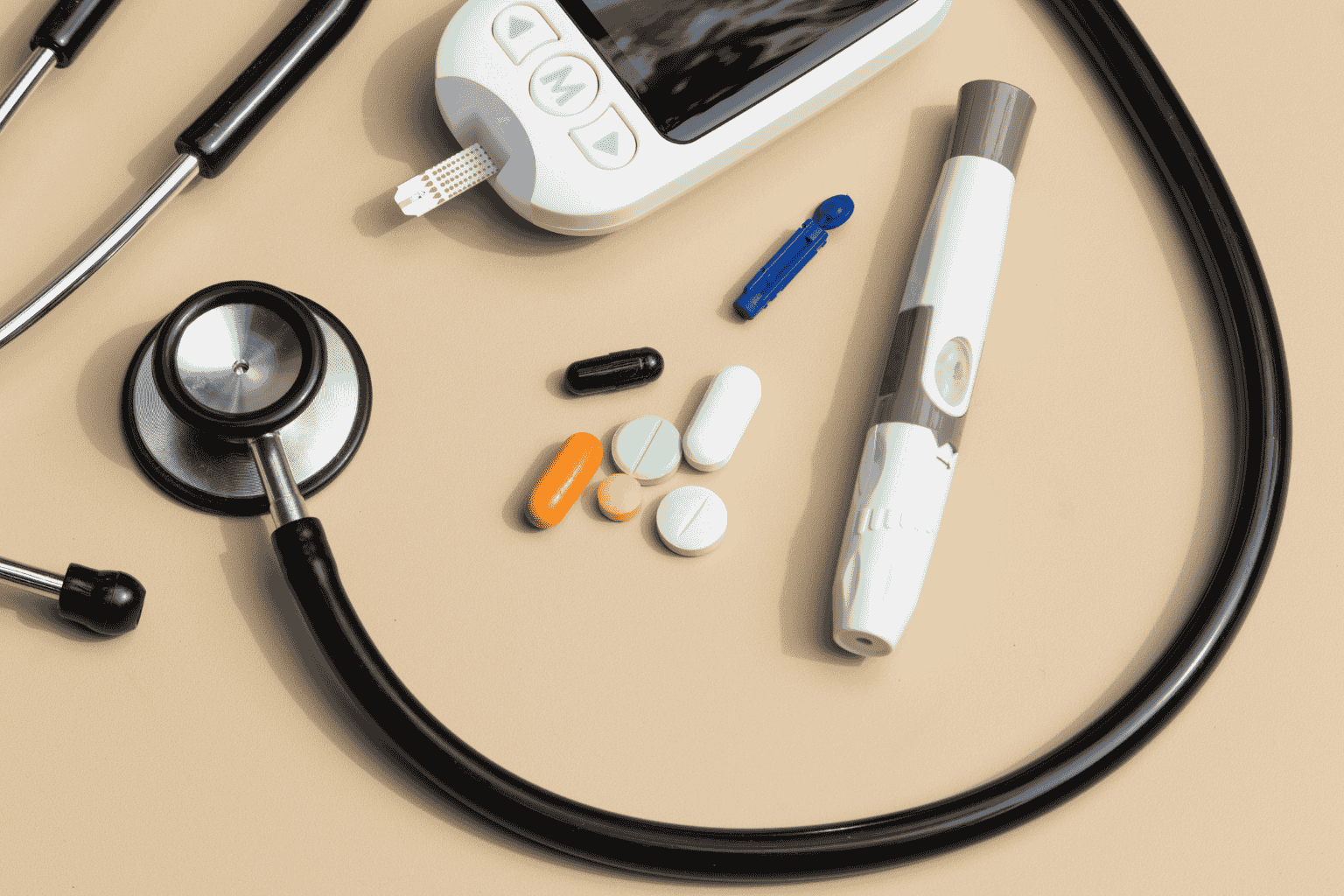
Diabetes affects nearly one in four care home residents, yet effective management extends far beyond simply checking blood glucose levels. Comprehensive diabetes care requires holistic approaches addressing medications, complications, foot health, nutrition, and emergency preparedness.
Understanding what truly excellent diabetes care looks like empowers families to ensure their loved ones receive the complete support this complex condition demands.
Why Diabetes Management Is More Complex in Care Homes
Elderly residents with diabetes face unique challenges that younger diabetics don't encounter: multiple chronic conditions requiring careful medication balancing, cognitive decline affecting symptom recognition, reduced appetite with unpredictable eating patterns, increased vulnerability to blood sugar complications, and communication difficulties preventing symptom expression.
These complexities mean diabetes care requires vigilant monitoring and responsive medical support beyond routine blood sugar checks.
Hypoglycemia: The Hidden Danger
Low blood sugar (hypoglycemia) is often more immediately dangerous than high readings, particularly in elderly residents.
Critical considerations:
Symptoms like confusion, sweating, shakiness may be missed or attributed to other causes
Severe hypoglycemia can cause falls, seizures, or loss of consciousness
Some medications cause unpredictable blood sugar drops
Residents with dementia cannot reliably report feeling unwell
Care staff must recognize subtle signs and respond immediately. Out-of-hours GP support ensures medical guidance is available when hypoglycemic episodes occur outside traditional surgery hours, preventing dangerous treatment delays.
Medication Management Beyond Insulin
Modern diabetes treatment involves complex medication regimens requiring expert oversight.
Common diabetes medications and considerations:
Metformin: Can cause digestive issues and requires kidney function monitoring
Sulfonylureas: Increase hypoglycemia risk, particularly problematic in elderly
Insulin: Requires precise dosing, proper storage, and injection technique
Newer medications: Monitor for dehydration and urinary infections
Regular GP medication reviews ensure treatments remain appropriate as health status changes. Same-day prescription delivery prevents dangerous gaps when medications need changing urgently.
Foot Care: Preventing Devastating Complications
Diabetes-related foot problems are among the most serious yet preventable complications.
Essential foot care protocols:
Daily foot inspections by care staff
Proper nail care by trained professionals
Appropriate, well-fitting footwear
Immediate GP assessment of any cuts, blisters, or discoloration
Regular podiatry appointments
Reduced sensation means injuries go unnoticed, whilst poor circulation slows healing dramatically. Minor wounds can rapidly become serious infections requiring intervention. Doorstep medical tests can assess circulation and infection severity without stressful hospital visits.
Diet and Nutrition: The Challenging Balance
Dietary management requires balancing blood sugar control with adequate nutrition and quality of life.
Residents with dementia may refuse diabetic-appropriate meals, whilst reduced appetite means ensuring adequate calorie intake becomes challenging. Modern diabetes dietary approaches are more flexible than outdated restrictive models. Regular GP reviews ensure dietary plans remain appropriate, particularly when weight changes or eating patterns shift.
Cardiovascular and Vision Health
Diabetes significantly increases cardiovascular disease risk. Blood pressure control is as important as blood sugar management, alongside cholesterol monitoring and recognition of heart attack or stroke symptoms.
Vision problems also require attention: annual eye examinations screening for diabetic retinopathy, monitoring for cataracts, and ensuring glasses prescriptions remain current. Vision problems affect mobility, increase fall risk, and reduce quality of life.
Emergency Preparedness
Diabetes emergencies require immediate recognition and response.
Essential protocols:
Staff trained to recognize and treat hypoglycemia immediately
Glucose tablets or gels readily accessible
Clear escalation procedures for unresponsive residents
Out-of-hours GP support for urgent medication guidance
Private ambulance services for rapid hospital transfer when needed
The Role of Comprehensive GP Support
Effective diabetes care requires accessible, expert medical oversight: regular comprehensive reviews (not just blood sugar checks), medication adjustments responding to changing needs, coordination with specialists when complications arise, and weekend and evening availability when urgent issues develop.
Onsite GP visits allow thorough assessments in familiar environments, whilst telehealth consultations provide convenient follow-ups and medication reviews.
The Bottom Line
Diabetes care in care homes demands comprehensive approaches extending far beyond blood glucose monitoring. Effective management requires attention to medications, foot health, cardiovascular risks, nutrition, and emergency preparedness —all coordinated through accessible medical support.
Care homes with robust GP partnerships offering regular reviews, out-of-hours support, and integrated services like same-day prescriptions and doorstep diagnostics can manage diabetes effectively, preventing complications and maintaining quality of life. Your diabetic parent deserves this complete, coordinated approach to their complex condition.


